Healthcare generates heaps of data every day. In fact, through 2025, there will be a 36% increase in healthcare data. This data can be from a multitude of sources like electronic health records (EHRs), wearables, and various medical devices. However, as John Baer said, “We are surrounded by data, but starved for insights,” which makes more sense for the healthcare sector. Why?
Think of a patient whose medical history is in one system, lab results in another, and their prescriptions in some other system. Either you’ll need to browse through all these systems to get hold of the records or rely on the respective departments to give a brief on it. Now, imagine this for thousands of patients every day. How frustrated would you be in offering tailored patient care through disconnected information?
Despite this, even if you get all the information, only a little piece of the data is effectively captured, analyzed, and utilized for optimal outcomes. Now, do you agree with John Baer?
Well, where there is a problem, there is a solution. Here is where Healthcare data integration comes in.
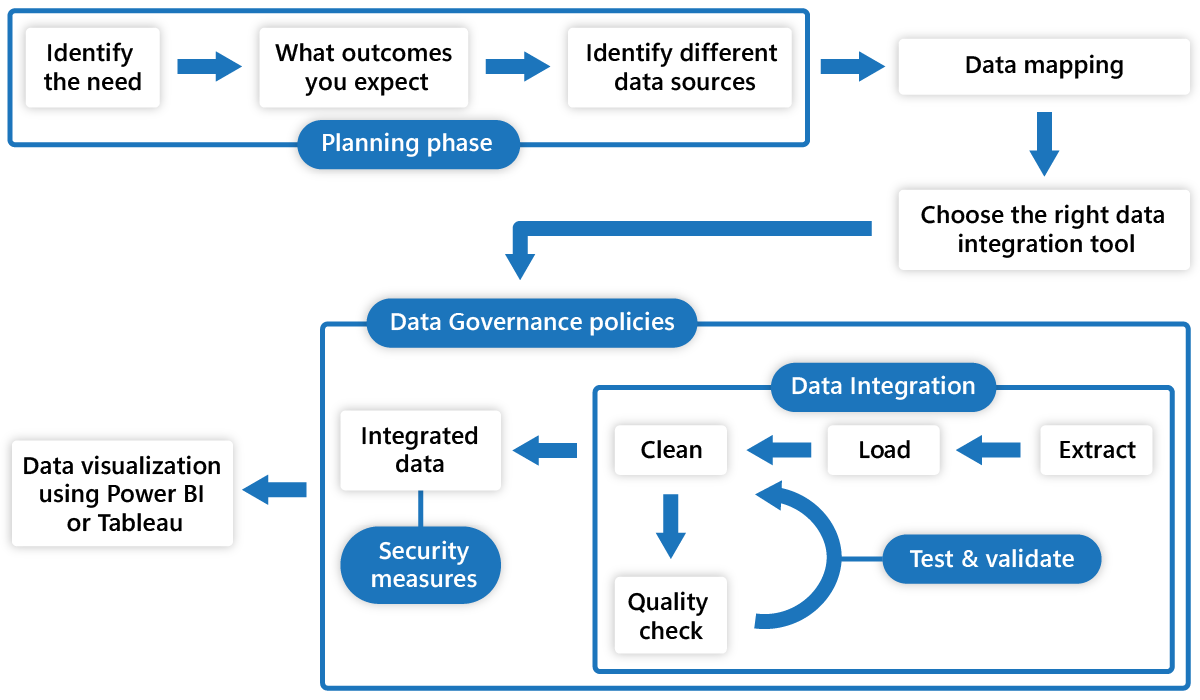
Fig. Healthcare data integration process
Healthcare data integration integrates all medical data from various disjoint sources into a single, unified platform to process and make it more usable for better decision-making.
To integrate data in silos, you must:
- Ask yourself- “Why do you want to integrate?”
- Next, ask- “Which data sources would you integrate for your goals?”
- Find the relation between different data
- Pick the apt integration tool suiting your technical infrastructure.
- Start extracting data from the identified sources, keeping the data relationships in mind.
- Load the extracted data into a central hub.
- Clean the data
- Run a quick quality check to ensure the cleaned data is error-free.
- Adhere to data governance policies throughout the process.
- Implement robust security measures to protect your patient information.
- Continuously test and validate for better accuracy and accessibility.
- Have role-based access to your integrated data.
- Train your relevant stakeholders in integrated data usage.
- Keep monitoring this solution for quickly resolving issues.
- Check that your data integration solution is scalable to handle future loads and flexible enough to handle updates.
- Get feedback to improve whenever necessary.
- Once integrated, use Power BI or Tableau to create visualizations and reports and make informed decisions.
However, implementation comes with its own challenges.
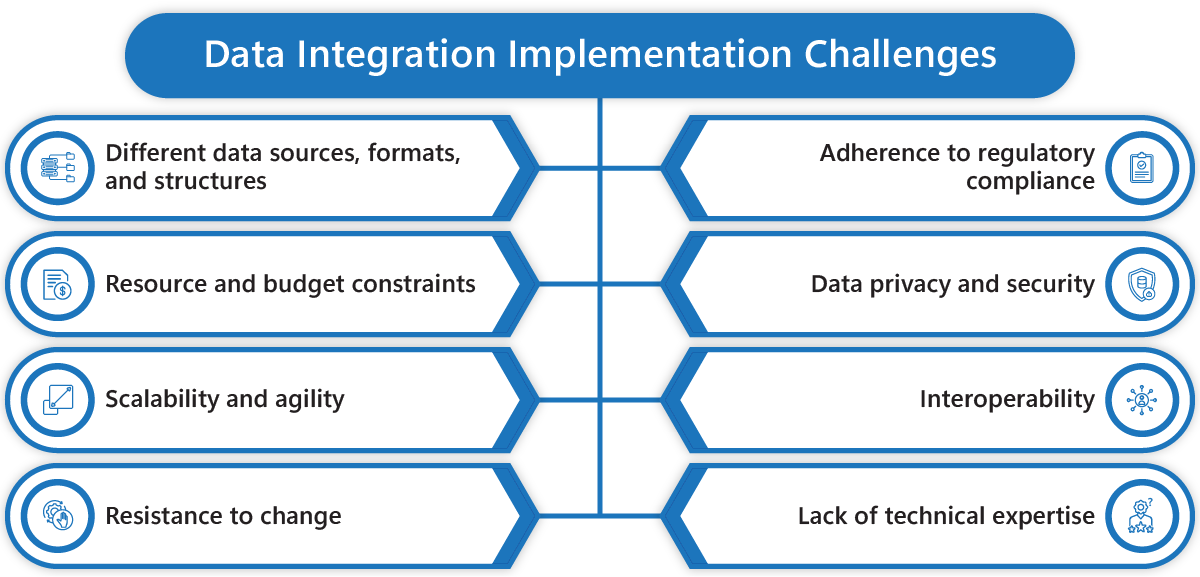
Fig. Challenges in data integration implementation
For example, integrating data from a wide array of sources is one of the challenges due to different formats and structures. Also, this data keeps coming in. Accommodating this ever-increasing data is yet another challenge for the healthcare sector. Is our system flexible enough to accommodate so much data pops up? Therefore, technology partners continuously strive to replace legacy systems with more advanced, high-performing, scalable systems.
Another challenge is interoperability while integrating data. As multiple healthcare applications use varied technologies and standards, ensuring data flow within such diverse systems is a hard nut to crack. Not just this, the data quality is also a matter of concern. Think of data having inaccuracies or errors. Can you use it for making decisions?
Healthcare works in a highly regulated environment. So, integrating data requires sticking around these regulations, seeming a distant goal at times. Also, patients subject their sensitive information to your organization. Ensuring the privacy and security of this information during the data integration process is quite a herculean task.
After navigating through all these challenges, healthcare professionals restrict themselves from adapting to these changes, posing another challenge. There can be reasons for resistance- lack of technical expertise, resource constraints, unwillingness to switch to new workflows, and lack of basic handholding.
So, shall you stop walking on the path of digital transformation? No.
With the problems, there are solutions to resolve them. To start with:
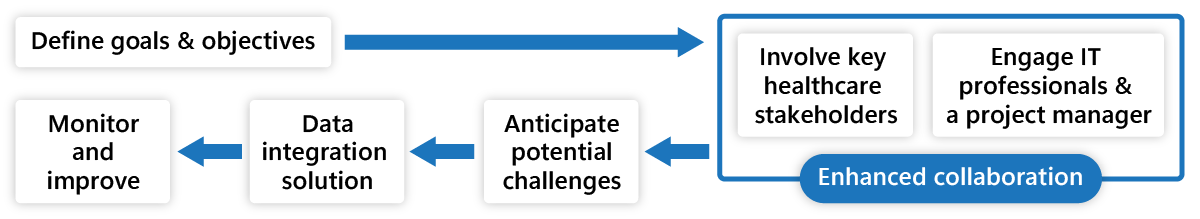
- Define your goals and objectives for data integration.
- Involve key healthcare stakeholders in the planning process to get clarity on the workflows and their desired outcomes.
- Anticipate potential implementation challenges, risks, and solutions in the planning phase.
- Assign an expert to handle your data integration efforts for both healthcare and IT.
- Engage IT professionals with expertise in data integration technologies and application development.
- Stay abreast of healthcare regulations and develop applications complying with them.
- Keep monitoring your systems and proactively identify and address challenges before they amplify.
- Collaborate with IT experts for seamless cross-functional operations and quick processes.
- Be agile with the plan.
- Finally, train your team using this integrated solution.
- Continuously evaluate and improve your solution with the decided parameters.
If you can implement data integration solutions successfully, you can get benefits like:
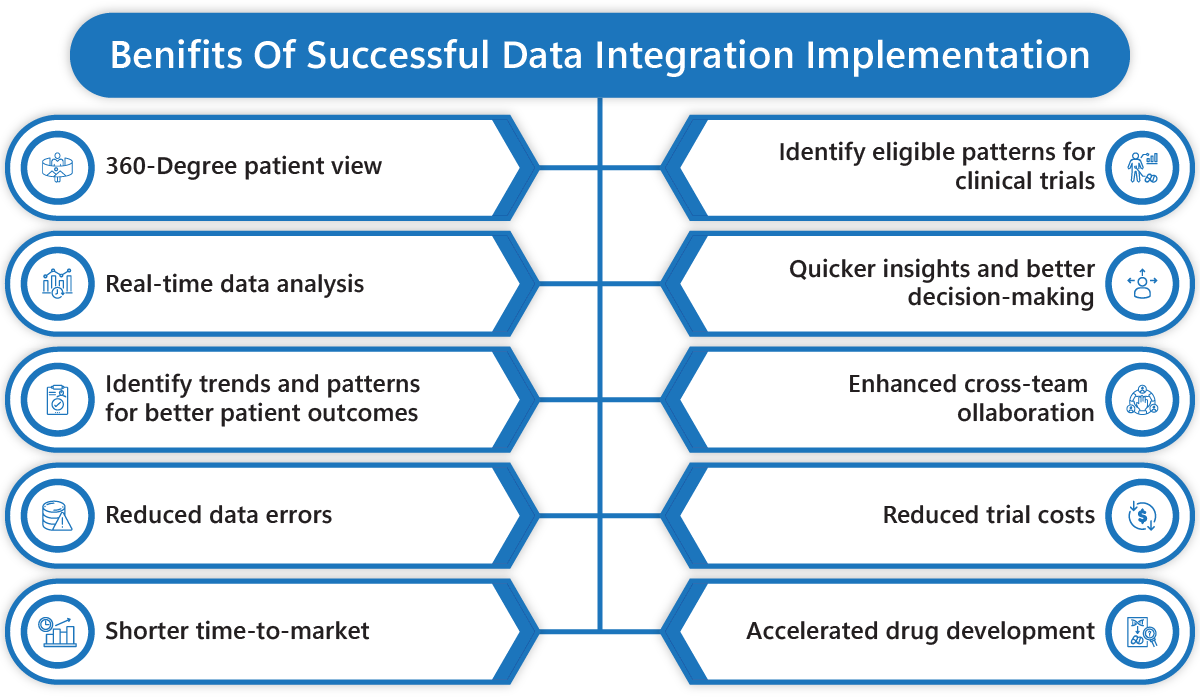
- A 360-degree view of your patient data for better understanding.
- Identify eligible patients for clinical trials.
- Real-time data analysis for quick insights and better decision-making.
- Identify trends and patterns for better patient outcomes.
- Reduced data errors and inaccuracies.
- Enhanced collaboration between healthcare teams
- Accelerated drug development.
- Reduced trial costs and shorter time-to-market for drug development.
Concisely, a data integration solution is your one-stop solution for getting a unified view of a patient’s medical history and a way to craft personalized treatments in the long run.
Nevertheless, partnering with a technology expert will bring massive benefits as they know how to address the potential challenges quickly and implement the solution aligning with your needs. So, whether you are a clinical researcher, hospital, or pharma company, your journey to become a data-centric organization starts with data integration. You are just a step away from crafting exceptional patient care. Now, it is on you- whether you want to capitalize on this opportunity quickly and get a competitive edge or allow the clock to tick, the choice is yours!
Top 6 FAQs on healthcare data integration
What is healthcare data integration?
- The process of integrating all the medical data from various sources into a single platform for a more unified view is healthcare data integration.
Why is data integration important in healthcare?
- With data integration, you can personalize your patient care and improve patient outcomes.
What are the steps involved in implementing healthcare data integration?
- Define integration goals
- Identify data sources
- Extract and load data into a centralized hub
- Clean the data
- Ensure compliance throughout
- Implement security measures on the integrated data
- Monitor and improve
What are the main challenges associated with healthcare data integration?
- Data from diverse sources
- Multiple data formats and structures
- Scalability to accommodate the massive volume of data
- Ensuring data flow within multiple applications
- Complying with regulations
- Resistance to change
- Budget and resource constraints
How can healthcare organizations overcome these challenges?
- Involving key stakeholders
- Anticipating problems to resolve before escalation
- Partnering with technology experts
- Collaboration with key experts to evaluate and improve the solution.
- Staying abreast of regulations
What are the benefits of successful healthcare data integration?
- Reduced trial costs
- Shorter time-to-market
- 360-degree view of patients
- Better patient care
- Real-time insights
- Better decision-making
